‘Routine’ Foramen Magnum decompression for Type I Chiari malformation
Case Presentation
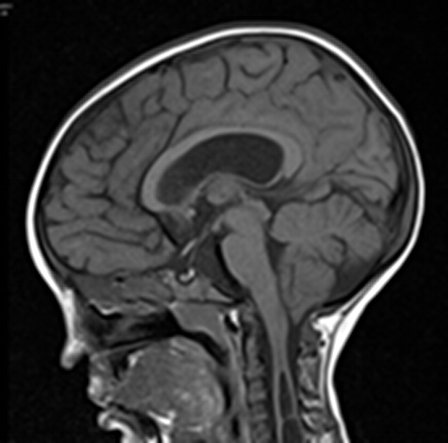
A 6 year old girl, who was previously diagnosed with Temtamy-Brachydactyly syndrome (growth retardation, talon cusps, sensorineural deafness, and bilateral symmetric abnormalities of hands and feet) was admitted with 3 months’ history of decreasing mobility, and brisk reflexes. An MRI scan (fig.1) revealed a Chiari malformation with extensive cervico-thoracic syringomyelia, signal changes in the right cerebellar peduncle, but with no hydrocephalus.

Fig 1
She underwent Foramen Magnum Decompression with duraplasty. The posterior arch of C1 was also removed, the dura was opened, and a duraplasty carried out with artificial dural substitute. A postoperative CT of head (fig. 2) done 2 weeks later showed bilateral subdural collections and a pseudomeningocoele at the operation site.

Fig 2
5 weeks after the operation, she presented with severe headache and vomiting. An emergency CT (fig.3) showed enlargement of the pseudomeningocoele with acute hydrocephalus.

Fig 3
An MRI (fig.4) showed adequate decompression at the Foramen magnum but persistent syrinx and the hydrocephalus, with features of raised pressure.

Fig 4
We debated whether to redo the foramen magnum decompression, or to insert a ventriculoperitoneal shunt and after discussion we decided to perform a shunt. The child has now improved and been discharged home following shunt insertion. We plan to repeat the MRI in 2 months to see the state of the syrinx, and the adequacy of the foramen magnum decompression.
Although the treatment of Chiari 1 malformation is theoretically straightforward, with foramen magnum decompression being the standard procedure, the complications may be considerable and may require further surgical intervention.

